News
Does the gut microbiota have a role to play in vaccine efficacy?
It is well established that the gut microbiota and immune system are inextricably linked; over half of all immunologically active cells in the body are located around the intestines.1 The gut microbiota is involved in the development and homeostasis of the immune system and a number of mechanisms have been identified for ways in which these microbes can influence both the suppression and promotion of viral infections.2
In response to the current viral pandemic, many research teams have been exploring the relationship between the gut microbiota, immunity and COVID-19 infections, which have been summarised in a review paper by Walton and colleagues.3
The review includes a pilot study comparing the gut microbiota of fifteen hospitalised COVID-19 patients to fifteen healthy controls, found significant alterations between the groups. Subjects with COVID-19 had elevated levels of opportunistic pathogens and a depletion of beneficial commensal bacteria. Furthermore, elevated levels of Coprobacillus species, Clostridium ramosum and Clostridium hathewayi were positively associated with COVID-19 disease severity.4
In a later publication, with a cohort of 100 COVID-19 patients, the same research group found significant differences again in the gut microbiota of patients compared to healthy controls. Specifically, they had reduced levels of Faecalibacterium prausnitzii, Eubacterium rectale and several bifidobacterial species – which are known to have immunomodulatory properties.5
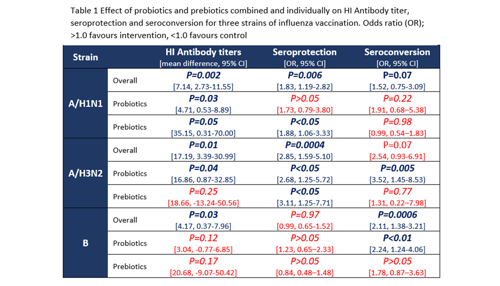
Walton et al. also explain that interventions targeting the gut microbiota have previously been shown to enhance the efficacy of the influenza vaccination.3 Although it is not yet known what effect dietary interventions could have on the COVID-19 vaccine, learnings from other viral vaccinations provide interesting insights. Meta-analyses exploring the effectiveness of probiotics and prebiotics on immune function after the influenza vaccination have found positive impacts on immunogenicity (hemagglutination inhibition(HI) antibody titers), seroconversion, and seroprotection, although this varies by the strain of influenza vaccine administered and the particular intervention (see Table 1).6,7
There is high heterogeneity between the studies included, such as the types of prebiotics and/or probiotics administered, but nonetheless, the results suggest that there is a potential role for dietary strategies targeting the gut microbiota to enhance effectiveness of influenza vaccination. It would be interesting to see further interventions exploring the potential of co-administration of prebiotics and/or probiotics alongside other vaccinations before any conclusions can be drawn from this research.
References
1. InformedHealth.org (2020) What are the organs of the immune system? [Accessed 26/01/2020] Available from: https://www.ncbi.nlm.nih.gov/books/NBK279395/
2. Li et al. (2019) Front Immunol 10:1551
3. Walton et al. (2020) Br J Nutr doi: 10.1017/S0007114520003980
4. Zuo et al. (2020) Gastroenterology 159 : 944-955
5. Yeoh et al. (2020) Gut doi:10.1136/ gutjnl-2020-323020
6. Yeh et al. (2018) Drug Des Devel Ther 12: 217-230
7. Lei et al. (2017) Nutrients 9(11): 1175
17/02/2021